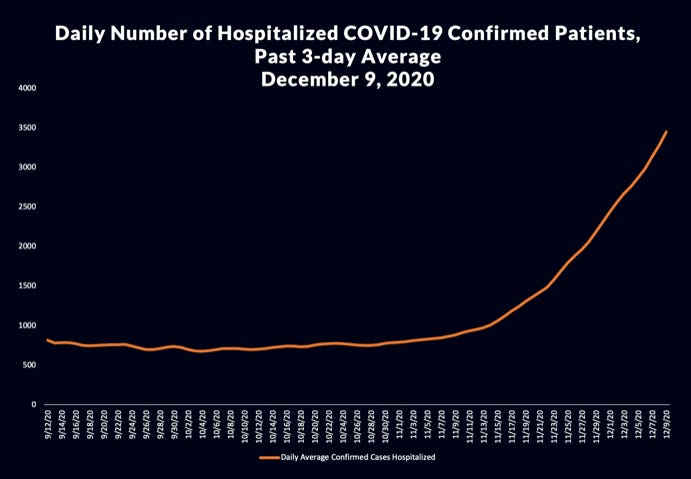
Sick and Tired – L.A. County Healthcare Workers Are Struggling As Cases and Hospitalizations Surge
I spoke to a chaplain that recently tested positive for COVID-19 and a nurse that has been on medical leave for two weeks and is returning to the biggest surge in coronavirus that the county has seen.
“The thing that has probably been the hardest and most heartbreaking has been the time I spend on the phone with families,” Joseph, a chaplain at an L.A. County based hospital told me on Friday afternoon, minutes before the L.A. County Department of Public Health reported a record breaking number of new COVID-19 cases for the second consecutive day. Over the past two days, the L.A. County Department of Public Health reported over 26,000 new cases of COVID-19 and over 100 deaths. As of Friday, 3,624 people were hospitalized for COVID-19.
Chaplain Joseph has witnessed three waves of coronavirus surges first hand, beginning with the initial surge in the spring and an additional surge in early summer. “This third wave is by far the worst thing I’ve seen.”
COVID-19 cases have increased over 1000% in the past month and a half. And hospitalizations have increased more than three fold since early September. Deaths are likely to increase in the next two weeks and officials say we could reach over 7,000 hospitalizations before the end of the month.
The recent surge in numbers doesn’t surprise Joseph though: “You see all different kinds of staff just disappear for two weeks.” He says healthcare workers at his hospital call it the “COVID vacation” or the “not good vacation.” This week over 1,700 healthcare workers and first responders tested positive for the coronavirus.
Joseph is currently on “COVID vacation.”
This past week, Joseph, his partner and their son all tested positive for the virus. Joseph is unsure if he contracted it from the hospital or elsewhere (his son also works as a grocery store clerk.) “Contact tracing is almost impossible at this point,” Joseph told me.
When he was at work, Jospeh spent most of his time talking to coronavirus positive patients virtually as well as family members of patients over the phone. Due to safety measures, family members aren’t able to be with their loved ones, even if they’re on the verge of death. “It’s just devastating, I’ve had families beg me and say ‘I don’t care if I die getting the virus, I just want to see my dad or my son one more time.’” The risk is too great though. “We’re doing the best we can and that has to be enough because there’s nothing else we can do,” Joseph told me when I asked how how his work has been impacted. Connecting with patients virtually isn’t ideal but there is no alternative. “We process our grief by being with people while they’re dying.”
As a former hospice care worker, Joseph was exposed to death regularly. “I’m fairly used to seeing death but I suspect that most nurses are not.” Joseph told me there was an emergency room nurse at his hospital that told him that for two months straight, every single shift that she work someone died, which she had never experienced before. “I do think there is going to be a mental health crisis.” Joseph says that his hospital is seeing more attempted and successful suicides than ever before.
To manage his own mental health, Joseph regularly sees a trauma therapist but he worries about how some nurses and first responders are managing the “secondary trauma” that they’re exposed to on a daily basis. Secondary trauma is defined as indirect exposure to trauma through a firsthand account or the narrative of a traumatic event. “The nurses are genuinely overwhelmed.”
On Friday evening I spoke to Cara, a clinical nurse that works at a hospital on the Eastside of L.A. County. Since Thanksgiving, Cara has been on medical leave, anxiously awaiting her return back to work this weekend. The public health crisis is changing so rapidly, Cara never knows exactly what she’s going to walk into when she arrives at work.

“1 o’clock every week day has been a beacon point in my mind because I realized that’s when the Public Health Department started releasing [case information]. I would start refreshing everyday on the DPH website to find out what the cases were looking like.” Recently Cara went back and looked at the press releases from the health department beginning in March. At the start of the pandemic we were only seeing dozens of cases and as more testing and data became available it was easier to see how cases would flatten out eventually. “This week they’re not flattening. It’s really scary.”
Since people like Chaplain Joseph are no longer able to come on the floor, even more responsibility falls on nurses. Nurses have to provide physical care but also emotional care for patients. Under normal conditions, Cara tells me that it’s easier to track patients physical progress. But with coronavirus, there are limited treatments available. “After the initial slate of Remdesivir (an anti-viral mediation), IV vitamin C and steroids, you can’t really do anything else. And if their respiratory function isn’t drastically improving or drastically decreasing, they’re just kind of holding and eventually what ends up happening is either one day they start getting a little bit better or they crash and it’s just kind of over. It’s not predictable in the same way [as other viruses] and you can’t measure improvement as drastically day-to-day as you can with other types of pneumonia.” Cara heard that there is a “freezer morgue truck” on site but she hasn’t seen it. Later in our conversation though, Cara said that being admitted into the hospital isn’t necessarily a death sentence. There’s a spectrum of different responses to treatment.
“It’s a really sinister virus.”
In April three people in Cara’s unit got exposed to coronavirus and all three ended up in the hospital (one person ended up in the ICU.) But now, all of them are back at work, “it took 5 months for them to be able to come back because they had to go home on oxygen.” One of Cara’s co-workers that got sick had been her charge nurse for a whole year, “all of a sudden I’m hearing about him in rounds and how he’s doing. Just hearing about him like you would a normal patient. It’s kind of hard to reconcile.”
According to Cara, there are currently three dedicated non-ICU COVID units and two ICU COVID units in her hospital. To staff all of the beds, the hospital is reportedly pulling administrative staff back onto the floor. According to Cara, nurse managers–staff that are in charge of a whole unit–have been putting in 18-20 hour days for weeks. “They have to but you can’t maintain that.” When I ask Cara how she manages her mental health, she tells me it’s been tough but acknowledges that there is a culture of pushing through difficult times amongst healthcare workers. “I think health care workers have a sense that ‘I do this job because of who I am as a person.’”
There is hope on the horizon though. On Friday, the FDA approved Pfizer’s COVID-19 vaccine. L.A. County is expected to receive approximately 83,000 doses by early next week, half a million doses before the end of the month and a quarter of million doses every week after that, if all goes to plan. Healthcare workers like Cara and residents of long-term care facilities will be the first group of people to receive the vaccine. “I’m so excited. I want all of them,” Cara joked. “Make me a test subject.” When I tell Cara that the health department cited a study that said that 60-70 percent of responders were undecided about taking a vaccine she said, “that gives me a pit in my stomach,” but doesn’t surprise her. Some people are afraid of the side effects, like one of her co-workers. “We know the side effects of COVID,” said Cara.
Today is the second day of Hanukkah and Christmas is in less than two weeks. As we approach more holidays, health officials are concerned that we may see another spike in COVID transmissions. Officials described the possibility of another holiday surge as potentially “catastrophic” on Friday. Earlier this week L.A. County Director of Public Health, Dr. Barbara Ferrer, said that we need to go back to how things were in the spring and early summer when very few people were on the sidewalks and streets.
Given the recent increase in hospitalizations, for frontline workers like Cara, it’s frustrating to see so many people disregarding health orders. “I think back to March when nobody was leaving their homes and everything was tainted with fear. Versus now when the need is now actually very dire–where as in March it wasn't–but non-essential retail is still open now.” Cara says she has an urge to go up to people that she suspects are congregating with groups of people outside of their household but “the social norms don’t lend themselves well to doing something like,” Cara says as she breaks out into laughter during an emotional conversation. “But at the same time what is public health if we’re not in everybody’s business about it. This is a group responsibility, this is not an individual thing, even though the government tells us it is.”
We might be able to see the light at the end of the tunnel but the repercussions of the pandemic will likely have long lasting impacts on communities and individuals. Chaplain Joseph calls the pandemic a “lifetime event,” it’s an experience that will effect all of us for the rest of our lives in some way. “There’s going to be a lot to unpack for a very long time.”
Lexis-Olivier Ray is an artist and writer based in Los Angeles as well as a regular contributor to L.A Taco, an award winning daily news publication known for its street-level reporting.
Enjoy my writing? Consider following me on Twitter!
Want to support my work? Feel free to buy me a virtual beer!
*Please contact me privately for corrections.